Favourable Effects of Vitamin D in Chronic Heart Failure – VINDICATE
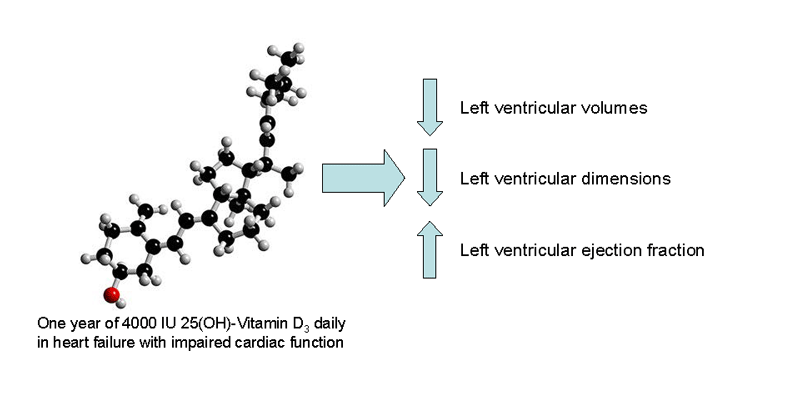
Favourable effects of vitamin D on cardiac function in patients with chronic heart failure secondary to left ventricular systolic dysfunction – the results of the MRC-funded VINDICATE Study
A daily dose of vitamin D3 improves heart function in people with chronic heart failure, a five-year University of Leeds research project has found. Dr Klaus Witte, from the Leeds University School of Medicine and Leeds Teaching Hospitals NHS Trust, led the study, known as VINDICATE, and here share his thoughts with us and our heart failure community.
“This is a significant breakthrough for patients. It is the first evidence that vitamin D3 can improve heart function of people with heart muscle weakness – known as heart failure. These findings could make a significant difference to the care of heart failure patients,” said Dr Witte.
Chronic heart failure is due to reduced pumping function of the heart and affects about 900,000 people in the UK and more than 23 million worldwide. The condition can affect people of all ages, but it is more common in older people – more than half of all people globally with heart failure are over the age of 75.
The most frequent cause of heart failure is heart muscle damage following a heart attack although high blood pressure, heart valve problems and infections can also lead to heart failure. The weakness is reflected by symptoms of shortness of breath and fatigue. Despite very good therapies including tablets and in some patients special pacemakers, many people with heart failure have persistent symptoms, and the heart muscle weakness remains.
“We found that almost all patients with heart failure in Leeds were deficient in vitamin D and that the degree of deficiency related to markers of severity. Vitamin D3 levels are largely dependent upon exposure to sunlight, yet levels are low throughout the year because heart failure patients are often older, spend less time in the sun, and also make less vitamin D3 in response to sunlight than younger people. Vitamin D3 production in the skin is also reduced by sunscreen.”
Vitamin D is known to have bone strengthening effects by improving calcium deposition in the skeleton, yet the substance is involved in many other systems, including muscle contraction, immune function, and insulin release, all of which may be abnormal in patients with heart failure. Up until now, there were no data suggesting that replacing vitamin D has any benefit in patients with heart problems.
The study, which was funded by the Medical Research Council, involved more than 160 patients from Leeds who were already being treated for their heart failure using proven treatments including beta-blockers, ACE-inhibitors and pacemakers.
Participants were asked to take 4,000 IU [100 μg] vitamin D3 or a dummy (placebo) tablet daily for one year. Those patients who took vitamin D3 experienced an improvement in heart function which was not seen in those who took a placebo.

Changes in heart function were measured by cardiac ultrasound (known as an echocardiogram). This allows us to measure how much blood pumps from the heart with each heartbeat, known as ejection fraction. The ejection fraction of a healthy person is usually between 60% and 70%. In heart failure patients, the ejection fraction is often significantly lower – in the patients enrolled into the VINDICATE study the average ejection fraction was 26%. In the 80 patients who took Vitamin D3, the heart’s pumping function improved from 26% to 34%. In the others, who took placebo, there was no change in cardiac function.
“One key aspect of this study is that we avoided using a calcium-based supplement, as calcium can cause further problems for heart failure patients. Crucially, the tablets were well tolerated by our patients and we saw no important side effects on kidney function.”
The findings from the VINDICATE study were presented at the American College of Cardiology 65th Annual Scientific Session & Expo in Chicago on April 4, 2016.
“In conclusion, we have shown for the first time that a high dose of vitamin D taken daily is safe and improves heart function in patients with heart failure. The next step is to use the information from this study to find out if improving the heart function reduces hospital admissions and extends the life of patients with heart failure. To this aim we have submitted an application to the National Institute of Health Research in the UK for VINDICATE 2 which will involve 1278 people with heart failure across the country for 4 years. The team at Pumping Marvellous have provided valuable advice in the development of VINDICATE 2 so please check back here to hear about the status of our application and, if funded, the status of the trial,” said Dr Klaus Witte.

Dr Klaus Witte MD, FRCP, FESC, FACC Associate Professor and Consultant Cardiologist
NIHR Clinician Scientist
University of Leeds and Leeds Teaching Hospitals NHS Trust